Neurologists and urologists have the highest rate of burnout among specialists, with almost two thirds of trainees reporting symptoms, according to a US study.
Researchers from the Mayo Clinic sought to explore the factors associated with career regret and burnout in a group of 3588 specialist trainees from 49 medical schools, who were surveyed during the fourth year of medical school and during their second year of graduate training residency.
Almost half (45%) of the doctors – representing 20 physician and surgical specialties – reported the symptoms of burnout, defined as a syndrome driven by work-related stressors such as emotional exhaustion, depersonalisation and a low sense of personal accomplishment. Burnout was associated with higher frequency of medical errors, problematic alcohol use and suicidal ideation, according Dr Lisolette Dyrbye and her co-authors of the study in JAMA.
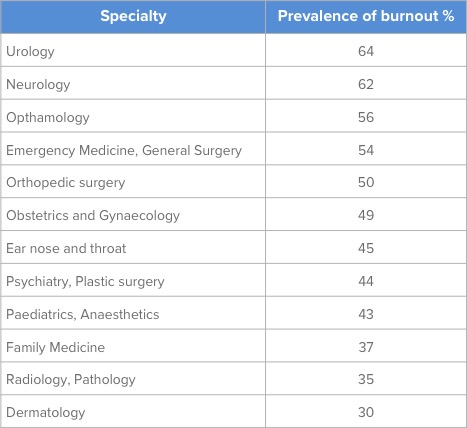
Source: JAMA September 2018, Vol 320 number 11
Their study assessed doctors using two questions from the Maslach Burnout Inventory;”I feel burnt out from my work” and “I’ve become more callous toward people since I started this job.”
The top three specialities with the highest prevalence of burnout were urology (63.8%) neurology (61.6%) and ophthamology (55.8%).
Specialties with the lowest rates of burnout were dermatology (29.6%), pathology (34.7%) and radiology (35.4%)
Burnout was more common in women than men (risk difference 7.2%) and in those who had reported higher levels of anxiety, and lower levels of empathy when they were in medical school.
The prevalence of burnout symptoms among residents was similar to that of practicing physicians, and much higher than the 28% average across US workers in other industries, the authors noted.