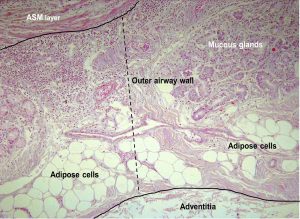
adipose tissue in the airways
Fatty airways could be contributing to problems with respiratory function in overweight and obese people, according to new research led by a WA team.
A study of cross-sectional tissues samples from postmortem lungs has demonstrated adipose tissue accumulates within the airway wall.
The deaths were categorised into three groups: non-respiratory deaths in people with no history of respiratory disease (controls), non-respiratory deaths in people with a history of asthma (non-fatal asthma), and asthma deaths (fatal asthma).
Samples from 1,373 airways from 52 lungs showed the fatty tissue was predominately in the outer wall of medium to large sized airways and seldom observed in small airways.
Adipose tissue was positively correlated with BMI in all three case groups.
Only BMI and male gender were found to be independently related to the area of airway adipose tissue.
The study, published in the European Respiratory Journal, provides the first evidence that fat accumulates in the lungs of overweight and obese people.
Previously, the increased prevalence and severity of asthma in people with obesity had been attributed to reduced lung volume due to thoracic compression or an inflammatory effect from adipose tissue.
“These results support a new mechanism of increased airway wall thickness associated with increased BMI which may contribute to excessive airway narrowing and exacerbate symptoms in patients with existing disease,” the study said.