Neurology is among the most demanding of specialities when it comes to mental, physical and time burden contributing to doctor burnout, researchers say.
A US study, based on national data from more than 5000 specialist doctors collected in 2018, calculated physician task load (PTL) scores for 23 distinct specialties with neurology scoring in the ‘red zone’ for mental demand.
Overall, neurology ranked around average for overall task load, due to having a lower burden on time and physical effort compared to other specialities such as emergency medicine.
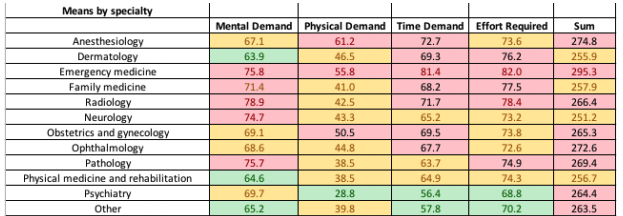
Emergency medicine recorded the highest task load total of 295.3 out of a possible 400.
Neurology (256.7) and dermatology (255.9) and both sat toward the middle of the range, ranking closely alongside family medicine (257.9), ophthalmology (255.7), pathology (255), and orthopaedic surgery (253.7).
Psychiatry (224) recorded the study’s lowest score, while urology (290) and anaesthesiology (274.8) placed second and third highest respectively sitting well above the mean score of 260.9.
 The authors of the study, published in the Joint Commission Journal on Quality and Patient Safety, identified a strong association between PTL and burnout.
The authors of the study, published in the Joint Commission Journal on Quality and Patient Safety, identified a strong association between PTL and burnout.
While the direction and possible causality of the association were both elements requiring further examination, they wrote, the relationship between the two suggested “areas of particular focus to improve the practice environment and reduce physician burnout”.
“Even a modest decrease in PTL was associated with a decrease in burnout, suggesting standard process improvement has the potential to positively impact PTL when looked at using this lens,” the authors wrote.