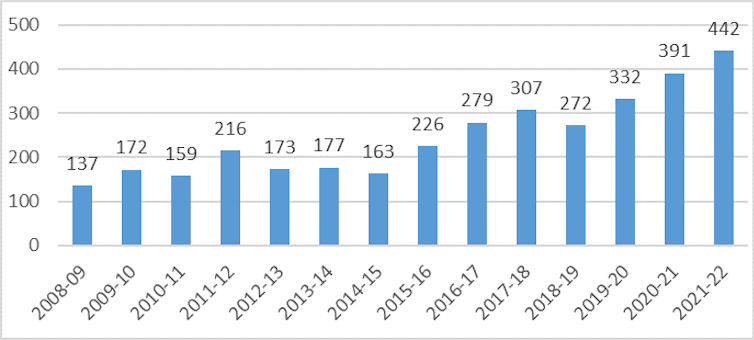
In 2022, 442 Irish doctors were issued with temporary work visas for Australia. This is a significant number of doctors compared with the total that Ireland trains each year (725 graduated in 2021).
Ireland has a long history of doctor emigration. UK research estimated that 71% of Ireland’s medical graduates of 1950-66 had emigrated by 1969. There was little interest in measuring doctor emigration back then, and little has changed in the past half a century.
Disinterest in doctor emigration stems from the belief that emigrant doctors will return and that doctor emigration will benefit Ireland.
Although emigrant doctors who returned with skills and experience obtained abroad have greatly enhanced Ireland’s medical training capacity, it is also important to acknowledge that doctor emigration without return has drained medical talent from the Irish health system.
Ireland has focused on the positive effect of doctor emigration and this has led to the development of a culture of medical migration. Although not unique to Ireland, such a culture accepts international training as inherently superior and requires doctors to complete additional training abroad (in the form of a fellowship) to further their careers. This means that in many specialities in Ireland, emigration is essential rather than optional.
When Ireland entered recession in 2008-09, the rate of doctor emigration increased, Australia emerged as a key destination, and doctors also began to emigrate earlier in their careers.
To better understand doctor emigration from Ireland, I began to study it.
In a survey of 307 emigrant doctors in 2014, I found that many had emigrated to escape difficult working conditions in the Irish health system. Emigrant doctors were enjoying the opportunity to work abroad in better-resourced health systems with superior working conditions. This both vindicated their emigration decisions and complicated their plans for return. As one doctor put it: “It’s awful to feel exiled from your country because of the expectations and work conditions of your job.”
Among those doctors surveyed, only one in four intended to return to Ireland. And the decision to return was for personal rather than professional reasons – for instance, to be closer to family and friends.
In 2018, I interviewed 40 Irish hospital doctors who had moved to Australia in the previous decade to find out why they had emigrated and whether they planned to return.
Unsustainable ways of working in Ireland also led them to decide to emigrate. They described Irish hospitals as understaffed and overstretched workplaces within which extreme ways of working had become normal.
In contrast, they enjoyed working in the Australian health system, describing well-staffed hospitals in which they were supported in their roles. Many had rediscovered their love of medicine while working in an efficient, well-resourced health system in Australia.
Once again, only a minority of those interviewed (one in three) planned to return to Ireland, indicating the risk of non-return inherent in all emigration decisions.
And then came COVID
However, this research was undertaken before COVID. Perhaps the pandemic changed the dynamics of doctor emigration.